Health
Ear health and hearing loss
10 times more Aboriginal than non-Aboriginal people suffer from ear diseases and hearing loss, most of them children. Aboriginal ear and hearing health is in crisis.

Wishing you knew more about Aboriginal culture? Search no more.
Get key foundational knowledge about Aboriginal culture in a fun and engaging way.
This is no ordinary resource: It includes a fictional story, quizzes, crosswords and even a treasure hunt.
Stop feeling bad about not knowing. Make it fun to know better.
Selected statistics
-
14% - Percentage of Aboriginal people with a long-term ear and/or hearing problem in 2018-19. [1]
-
58% - Percentage of Indigenous children aged 0-14 years with poor ear health living in remote communities in Queensland. [2] Equivalent figure for 0-4 year-olds: 85%. In those years the auditory link with the brain develops.
- 4
- Times a child with hearing loss is more susceptible to sexual abuse. [2]
-
90% - Percentage of Aboriginal inmates at Darwin Correctional Centre with hearing loss [3]. Equivalent figure for male Aboriginal inmates in Alice Springs: 95%. [4]
- 10
- Times Aboriginal people suffer more from ear disease and hearing loss than non-Indigenous people. [3]
- 5..6
- Average age of first hearing aid fitting for Aboriginal children. [5]
- 32
- Average time in weeks Aboriginal children and young adults aged 2 to 20 years suffer from middle ear disease. Equivalent figure for non-Indigenous children: 2 weeks. [6]
-
7% - Percentage of Aboriginal children in remote communities with healthy ears. 93% of Aboriginal children suffer from middle ear infections in early childhood. In remote NT communities this ranges from 8% to 50%. The World Health Organisation regards 4% as a 'massive public health problem'.
-
95% - Proportion of male Aboriginal prisoners in Alice Springs prison who suffer from hearing loss. Same figure for Darwin: 92.5%. [7]
"Some have no ear drums at all": Aboriginal ear health is in crisis
20% of young Aboriginal children in the Northern Territory suffer from the most severe form of ear disease, chronic draining ears or burst eardrums. [8] This is in stark contrast with Aboriginal children in Nigeria (7.3%) and New Zealand's Maori children (4%). Ear disease was not a significant problem for Aboriginal people prior to colonisation. [9]
Recurrent infection leads to persistent ear discharge and perforated ear drums in 40% of Aboriginal children in remote areas before 18 months of age. Some have no ear drums at all. Urban rates are not as high, but still 3 to 4 times higher than in the non-Aboriginal population. [10]
A federal inquiry into hearing health repeatedly found a relationship between hearing loss and early Aboriginal justice problems [3] which limits life chances of the young Aboriginal generation in education, employment and justice.
With 10 times more Aboriginal people than non-Aboriginal people suffering from ear diseases and hearing loss, Aboriginal ear and hearing health is "in crisis". [3]
In a community in central Australia I visited, the health worker was baffled by a patient, a little girl. She called me over to have a look and it was a normal, healthy ear drum. She’d never seen one before.
— Dr Kelvin Kong, Aboriginal ear surgeon [10]
The final report of the Royal Commission into Aboriginal Deaths in Custody (1991) first noted the relationship between childhood ear disease, hearing loss and poor school performance, and their connection to involvement in the criminal justice system. [5]
Story: "Students are much happier"
A school in Meekatharra, about 760 kms north-east of Perth, Western Australia, was able to improve students' learning and behaviour when it introduced microphones and speakers in the classrooms. [11]
Teachers started to use the system in 2004 to enable all students hear instructions clearly. Amplifying the teacher's voice increased attentiveness and on-task behaviour of the students.
"The students are not getting frustrated or confused about what is being asked of them. They are much happier with themselves because of their results, their confidence increases daily," observes Toni Matthews, a Year 6/7 literacy and numeracy teacher.
Causes of hearing loss
Recurrent middle ear infections, or otitis media (OM), is the most common ear disease among Aboriginal children. In 2018-19, among children aged 0-14 years, 2.6% had otitis media and 3.8% were partially or completely deaf. [1]
The disease is typically caused by bacterial and viral pathogens. Research suggests that the viruses and bacteria were introduced from crowded European cities into the previously isolated Aboriginal communities, and that Aboriginal people had no immunity to the viruses. [9]
Secondary causes are
- poor health care (e.g. poor hand and face hygiene),
- smoking,
- poor diet, and
- crowded and unhealthy housing which facilitates transmission of bacteria.
A "second wave" of hearing loss is caused by persistent exposure to loud noise, especially in some home environments. As family members with existing hearing loss turn up the volume of TVs, radios and phones, or simply shout and scream to communicate, other members of the family suffer from excessive noise. [12]House parties can have noise levels similar to discos or concerts and go on for much longer. In remove communities long car trips are common, and loud music may be played for many hours – with people frequently shouting over the music to communicate.
Some of the trips are used to hunt and whole family groups are passengers. But when firearms are discharged at close hearing range of small children, repeated exposure causes permanent hearing loss.
In contrast, non-Aboriginal hard-of-hearing are fewer in number and mostly over 50 years old. They do not as often live with others with hearing loss, in large households, or with children.
Fact Stress is a major factor affecting health. Racism and disempowerment affect both physical and psychological health. Positive stories in the media, anti- racism programs and establishment of a treaty have been shown to have a positive effect on health in Maori and Native American populations. [9]
Video: How 'glue ear' (otitis media) develops
Ear disease affects every aspect of life

Can you believe that Aboriginal people have a greater chance of being locked up than non-Aboriginal people because they can't hear well?
Ear disease, hearing impairment and communication disorders along with the life-long otitis media (OM or glue ear) affect "exceptionally high" levels of Aboriginal children [2]. About 75-80% of all Aboriginal children have had at least one episode of Otitis Media by the age of five [13].
Ear diseases impair the development of talking and listening skills and reduce their ability to understand, follow and memorise what is being taught at school, leading to truancy, poor speech and performance at school. It affects self-esteem and behaviour, especially given some of Aboriginal children have English as a second or third language. [10]
Poor education leads to poorer employment and lower income, followed by lower living conditions and poorer health, thus completing a long-term cycle of a life of disadvantage. Overcrowding, poor diet, poor sanitation and passive smoking are other factors [3].
Aboriginal students with poor hearing participate less in classroom activities. Hearing problems lead to social exclusion which progresses to relationship breakdown, alcohol and drug issues, antisocial behaviour or a criminal career. As many as 80% of students have Otitis Media and associated hearing loss at some time during any school year, 10 times more than non-Aboriginal children [13].
From an early age, children are schooled in the practice of making 'tissue spears’' to soak up water after swimming and discharge caused by infection. [10]
Adults with hearing loss may experience more depression and cardiovascular disease [12].
Engagement between Indigenous people with a hearing loss and police can spiral into confrontation, as police mistake deafness for insolence, or for cultural or language communication difficulties.
— Rachel Siewert, chair, Senate Community Affairs References Committee [3]
Story: "A good cold can halve my hearing ability" – Living with hearing impairment
Celeste Liddle, an Arrernte Australian woman writing for the SMH and Guardian, and a National Indigenous Organiser, shares how her hearing impairment will affect her for the rest of her life [14].
"When I was about seven years old, I was sent to speech therapy. Over a few months, I worked with a therapist to correct patterns of discussion and counteract a well-developed mumble which I had acquired. In the years that followed, many people remarked on my comparatively refined 'accent' and are usually shocked when I tell them how I acquired it. So why then, as a child, did I mumble? It was because, like many Aboriginal children, years of chronic ear disease had left me speaking how I heard the words being said to me.
"While I had navigated the system educationally in these younger years so that somehow my writing and reading skills became quite advanced, I continually had issues grasping spoken instruction. This led to behavioural issues such as frustration and social withdrawal. I was beyond awkward and introverted. Speech therapy and the insertion of grommets was the beginning of what has been a lifetime of treatment for ear ailments. Even now, a good cold can halve my hearing ability for up to three weeks, tinnitus is a fact of life, and perforated ear drums are normal...
"Despite the fact that I will have ear problems for life and indeed am facing restorative operations and severe hearing loss later on, I am forever thankful that my issues were picked up and that I was able to access appropriate treatment as a child. This treatment allowed me to catch up to my peers at school as well as develop mechanisms to cope with my limitations. My focus on writing as a key communication mode is indeed a huge part of learning to work with these limitations. The likelihood of me eventually finishing school and going on to university would have been severely diminished had these problems not been addressed."
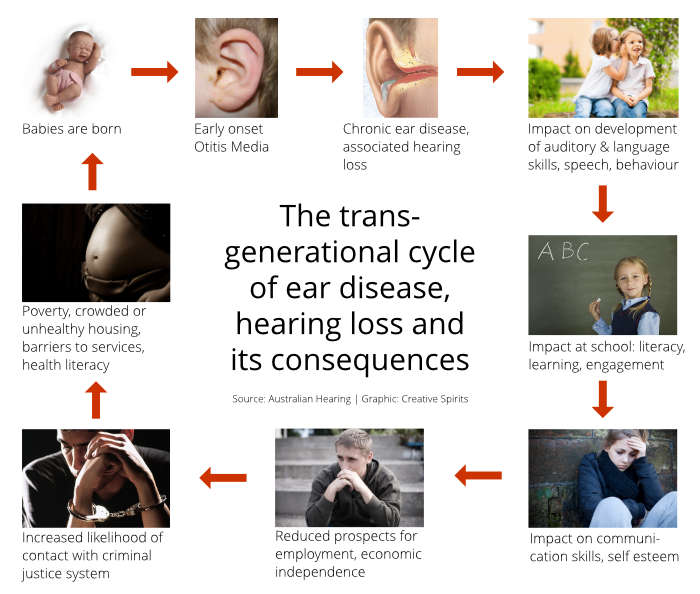
Less hearing = more jail time
There is a direct association between children diagnosed with language impairment through hearing loss at age 5 and later misconduct at age 19. [9]
The typical path is early onset ear disease > fluctuating hearing in early childhood > language impairment > lower school readiness > less school engagement & participation > ‘delinquency’ in adolescence > increased risk of engagement in criminal activity.
Aboriginal ear surgeon Dr Kelvin Kong tells the following story: "A guy came in who was 40 and he typifies all that’s wrong with ear health. He had what he described as noises in his ears and when we had a look there were maggots in there. This was in Newcastle, this wasn't remote Australia... It’s no surprise that as a consequence he couldn't read or write, was unemployed, in and out of prison." [10]
Hearing-impaired Aboriginal people attending court hearings have to second-guess what is being asked or said, letting them admit things they did not do. Suspects treated as defiant or non-compliant because they didn't respond to directions might simply not have heard them.
Hearing-impaired Aboriginal people are very prone to wrongful convictions. In 1961 a deaf-mute teenager was sentenced to death, but later to life imprisonment, because he made a false confession [7].
Hearing impairment has become "a significant disability in a custodial environment" [4], with evidence mounting that it is also an important component of Aboriginal disadvantage.Hearing loss is often more common among Aboriginal prisoners than for their non-Aboriginal peers.
Prison guards in the Northern Territory are now carrying amplification devices to deal with prisoners' hearing disabilities [7]. Schools have started introducing surround-sound systems to amplify teachers' voices in the classroom [15] (see also story below).
Police have a rule that disabled people must be given extra care, but abled speakers have difficulties relate to deaf and hearing-impaired people's different concepts and experience of life. Researchers demand greater translation support, such as a "hand talk" (community sign language) translator, an Auslan translator and a cultural advisor [7].
Imprisonment [of hearing-impaired Aboriginal people] in some instances would be equivalent to solitary confinement.
— Dr Damien Howard, Psychologist, Northern Territory [16]
The high prevalence of hearing loss among Aboriginal children points to it being an important factor in the high rates of abuse of Aboriginal children in Australia, says Damien Howard, psychologist in Darwin specialising in social and justice challenges faced by juveniles with a history of otitis media [2]. No formal research has been done.
A report found in 2015 that 55% of children who received services in 2013/14 suffered from hearing loss [17].
None of the welfare agencies involved in child protection have any awareness of the [poor ear health] issue, screen children, or consider it in their services or support.
— Damien Howard, psychologist, Darwin [2]
Getting hearing back
Poor diet is one factor for declining ear health. Many Aboriginal families, especially in remote communities, only shop for food once a fortnight or occasionally. They choose food they can keep in the freezer which excludes fresh fruits or vegetables.
When doctors supplied families with subsidised vegetables they watched students' hearing return, to the point that a formerly introduced amplification system could be abandoned, antibiotics cut down, and infections decline [15].
"It is very simple and was cheaper than buying antibiotics," said one doctor. "Antibiotics cost $100 for a bottle but 100 [dollars] buys you a lot of fruit."
The only hurdle to delivering more such programs is funding.
Edie Wright, a regional consultant for Aboriginal education in the Kimberley, implemented the 'BBC' program. Each morning, the kids would "breathe, blow and cough" and complete a set of exercises to enable postural drainage. "We reduced our ENT [ear, nose and throat] referrals by 70%,’’ she says. [10]
For others, the hearing damage is permanent. They need hearing aids.
Children need to hear well a long time before school starts. Sadly, the average age of first hearing aid fitting for Aboriginal children is 5 or 6 years, which is very late in relation to speech and language development and school readiness. [5] About 24% of non-Aboriginal children are fitted for the first time aged under one year, compared with only 5% of Aboriginal children. [9]
Modern hearing aids don't need to be 'uncool' and embarrassing. Doctors can fit a subtle device into a cap of the child's choosing which they have to wear in the classroom. [10]
Does it work?
A survey of 200 Aboriginal hearing aid-wearing adults from remote, rural and urban communities found that [5]
- 96% were ‘happy’ or ‘very happy’ with their aids,
- 86% enjoyed time with family and friends ‘a lot’ or ‘quite a bit’ more,
- 86% said they were ‘a lot’ or ‘quite a bit better’ at doing business for themselves,
- 75% said they did not feel shame when wearing their hearing aids.

Resources
Damien Howard has put together the Look After Kids' Ears website which has lots of resources about middle ear disease (sick ears or otitis media) and listening problems (hearing loss). It helps educators, teachers and families learn how to prevent kids from getting hearing problems.
The Queensland government is running the Deadly Ears Program for children. It aims to reduce the high rates of conductive hearing loss in Aboriginal communities and achieve long-term changes across the education, health and early years services.